Retrieval results
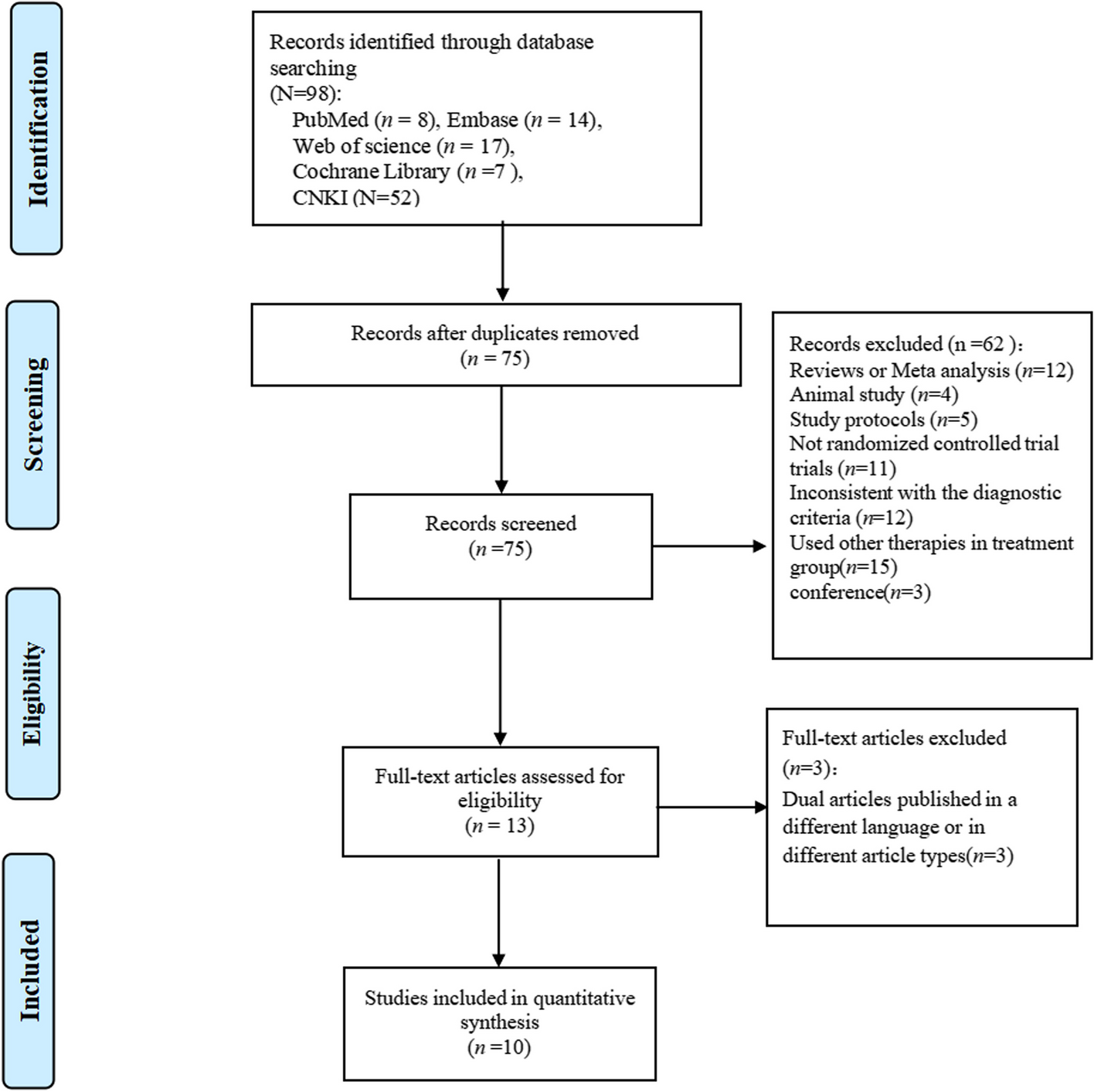
According to the literature search strategy, 98 articles were initially retrieved from five databases, including 8 articles in PubMed, 14 articles in EMBASE, 7 articles in Cochrane, 17 articles in Web of Science and 52 articles in CNKI. Second, a total of 65 articles were excluded by reading article titles, abstracts, and full texts. Two of the articles [23, 24] were the same study, but included different fMRI data. Ultimately, we included 10 studies (including 11 articles) [21, 23,24,25,26,27,28,29,30,31,32]. The process of literature screening based on PRISMA is shown in Fig. 1.
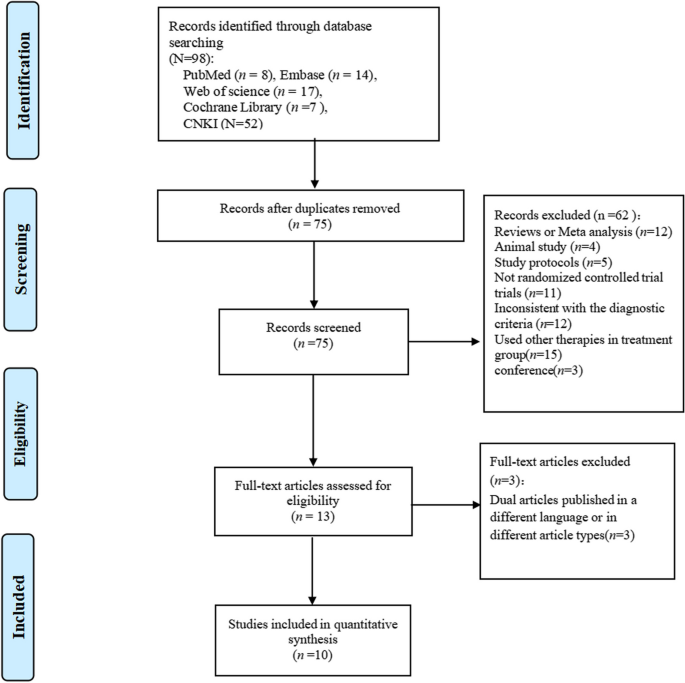
Article screening process
Study characteristics
This study ultimately included 10 RCTs, including 4 FD studies [21, 23,24,25,26], 3 IBS studies [27,28,29], and 3 FC studies [30,31,32]. All studies used the Roman diagnostic criteria, published from 2012 to 2021, and included a total of 474 participants, 406 of whom completed fMRI. All of the studies were from China, and six of them [21, 25,26,27,28,29] were published in English. The proportion of females in these participants was 10 to 97.1%, except for two studies not mentioned [27, 29]. The intervention measures in the treatment groups were acupuncture, including MA, EA and TEA. Six of the studies used sham acupuncture (SA) [21, 23, 24, 26, 28] or waiting for treatment [31, 32] as controls, and three used moxibustion [25, 27, 29] or medication (polyethylene glycol) as controls [30]. All studies reported the results of brain fMRI, of which three IBS [27,28,29] studies used event-related fMRI, and the rest used resting state fMRI. The acupuncture efficacy in FGIDs was reflected with certain gastrointestinal symptom scales in eight studies [21, 23, 24, 26, 27, 29,30,31,32], and anxiety and depression rating scales were put to use in five studies [21, 23, 24, 26, 27, 29] to assess psychological status. Detailed information of the included study characteristics is shown in Table 1.
Clinical outcomes
All studies reported brain imaging data results, and eight [21, 23, 24, 26, 27, 29,30,31,32] of the studies reported clinical outcomes, which were divided into two categories: FGIDs symptoms and psychological outcomes.
FGIDs symptoms outcomes
A total of 8 studies compared the FGIDs symptoms of patients after acupuncture treatment, including 3 FD studies [21, 23, 24, 26], 2 IBS studies [27, 29], and 3 FC studies [30,31,32]. Combined results showed that acupuncture could significantly improve the clinical symptoms of FGIDs patients, including abdominal pain, abdominal distension, frequency of defecation, and stool characteristics, etc.
FD symptom outcomes
In FD clinical trials, the most commonly used FD symptom assessment questionnaire is the NDI questionnaire [33], including the Nepalese Dyspepsia Symptom Index (NDSI) [34] and the Nepalese Dyspepsia Life Quality Iindex (NDLQI), which can record both FD symptoms and FD specific quality of life. In this systematic review, two studies used the NDI questionnaire [23, 24, 26], one study [21] used the NDSI score to evaluate clinical symptoms of FD.
The taVNS group could significantly improve the overall symptoms of FD and reduce the NDI score (both P < 0.05), while the sham-taVNS group only improved the overall symptoms [23, 24]. Our review showed that the clinical symptoms of FD improved after both acupuncture and sham acupuncture treatment (P < 0.05), and the MA Deqi group showed greater decrease of the FD symptom score than that in the MA without Deqi group (P < 0.05) [21, 26].
IBS symptom outcomes
Both IBS studies used Visual Analogue Scale (VAS) to assess major gastrointestinal symptoms, one in patients with IBS-C [27] and the other in patients with IBS-D [29]. Our results showed that after 4 weeks of treatment in IBS-C patients, the improvements in abdominal distension, defecation frequency, difficulty in defecation, and stool form were significantly greater in the EA group than in the MOX group (P < 0.01) [27]. After 4 weeks of treatment in IBS-D patients, compared with before treatment, the EA group reported significant improvements in abdominal pain, abdominal distension, defecation emergency and defecation frequency (P < 0.05 or P < 0.01), but the MOX group showed more significant improvements in emergency defecation and defecation frequency (P < 0.01) [29].
FC symptom outcomes
One of the results showed [30] that the PAC-SYM scores of the two groups (acupuncture vs. medication) of FC patients after treatment were significantly decreased (p < 0.01), while there was no statistical difference in the improvement of the PAC-SYM scores between the two groups (p > 0.05). Two other studies [31, 32] showed that the PAC-SYM and PAC-QOL (Patient Assessment of Constipation Quality of Life) scores of FC patients were significantly decreased after acupuncture treatment (P < 0.01 or P < 0.05). Among them, in Hou’s study [31], the improvement values of PAC-SYM and PAC-QOL scores in the acupuncture group were greater than those in the WT group (P < 0.05), while in Ma’s study [32], only the improvement in PAC-QOL score was greater than that in the WT group (P < 0.05).
The comprehensive results of the meta-analysis showed that acupuncture treatment could effectively reduce the PAC-SYM score in patients with FC. [MD = − 2.10; 95%CI (− 4.11, − 0.08); Z = 2.04; p = 0.04]. Subgroup analysis showed that compared with the WT group, acupuncture could reduce the PAC-SYM score of FC patients [31, 32] [MD = − 2.73; 95%CI (− 4.95, − 0.51); Z = 2.41; p = 0.02], but there was no significant difference compared with the medication group [30] [MD = 0.83; 95%CI (− 3.95, 5.61); Z = 0.34;p = 0.73] (Fig. 2).
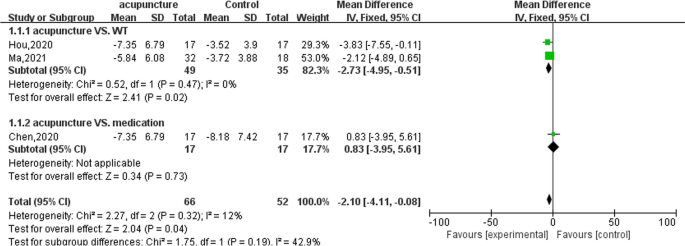
Meta-analysis of PAC-SYM of treatment group and control group
Psychological outcomes
Patients with FGIDs are often accompanied by psychological disorders. Therefore, anxiety and depression scores were included as secondary outcomes in this study. A total of 5 studies compared the psychological outcomes of patients with FGIDs after acupuncture treatment, including 3 FD studies [21, 23, 24, 26], 2 IBS studies [27, 29]. In our systematic review, Zung Self Rating Anxiety Scale (SAS) and Zung Self Rating Depression Scale (SDS) [21, 23, 26], Hamilton Anxiety Rating Scale (HAMA) and Hamilton Depression Rating Scale (HAMD) [23, 24, 27, 29] were used to evaluate psychological status. Combined results showed that acupuncture could significantly relieve anxiety and depression in FGIDs patients.
In FD patients [21, 23, 24, 26], both the acupuncture group and the sham acupuncture group had significantly decreased anxiety and depression scores after treatment (P < 0.05).Three studies [21, 23, 26] including 150 participants compared the SAS and SDS scores after acupuncture treatment in patients with FD. The heterogeneity test showed high heterogeneity (I2 = 98%, p < 0.00001; I2 = 86%, p = 0.0007), the randomized effect model was adopted.
The comprehensive results of the meta-analysis showed that there was no significant difference in SAS and SDS scores between the two groups in patients with FD [MD = 6.44; 95%CI (− 7.38, 20.25); Z = 0.91; p = 0.36]; [MD = 2.55; 95%CI (− 2.79, 7.88); Z = 0.93; p = 0.35]. Subgroup analysis showed that compared with the sham-taVNS group, taVNS could reduce the SAS and SDS score of FD patients [23] [MD = 17.90; 95%CI (17.30, 18.50); Z = 58.25; p < 0.00001]; [MD = 6.52; 95%CI (6.10, 6.94); Z = 30.13; p < 0.00001], but there was no significant difference between the MA group and the SA group [21, 26] [MD = 0.71; 95%CI (− 2.72, 4.14); Z = 0.40; p = 0.69]; [MD = 0.01; 95%CI (− 3.33, 3.35); Z = 0.01; p = 1.00](Fig. 3).
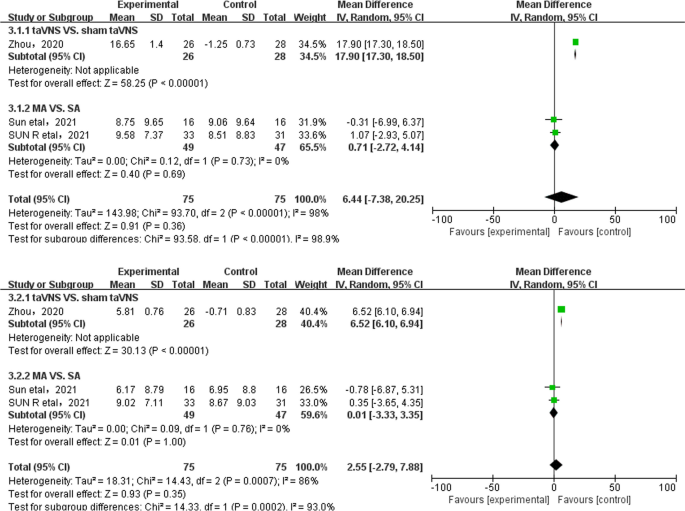
Meta-analysis of SAS/SDS of treatment group and control group
The IBS clinical studies included in this review all used moxibustion as the control group. IBS-C patients in the EA and MOX groups had significantly improved anxiety and depressive after treatment (P < 0.01) [27], and the improvements were significantly higher in the EA group than in the MOX group (P < 0.01), whereas in the IBS-D study, MOX treatment was more effective than EA treatment (P < 0.01) [29].
Central mechanism-brain imaging data
Acupuncture-related brain activities can be divided into four categories for summary and analysis: comparison before and after acupuncture treatment, comparison between acupuncture and sham acupuncture or no intervention groups, comparison between acupuncture and moxibustion groups, comparison between acupuncture and medication groups. The activation of the most frequently reported brain regions (temporal gyrus, insula, ACC, PFC, thalamus, HIPP, amygdala, posterior cingulate, etc) are summarized in Table 2.
Comparison before and after acupuncture treatment
Resting state fMRI before and after acupuncture treatment
After taVNS treatment for 2 weeks, the ALFF values in the left HIPP and left paraHIPP of the FD patients increased (P < 0.05) [23], the regional homogeneity (ReHo) values in the left middle temporal gyrus and left precentral gyrus (PrG) increased (P < 0.05) [24]. After 4 weeks of Zusanli (ST36) acupuncture treatment, the fALFF values in the right paraHIPP, left cerebellum, and left paraHIPP in FD patients were significantly increased (P < 0.01), and the fALFF values of the right middle occipital gyrus, right cuneus, left precuneus, left middle occipital gyrus, right superior frontal gyrus, left superior frontal gyrus, left inferior frontal gyrus, and the left superior frontal gyrus were significantly decreased (P < 0.01) [25]. After treatment of FD patients with acupuncture Deqi, the left BLA rsFC with right cuneus increased significantly, the left BLA rsFC with right HIPP and bilateral INS/putamen decreased significantly, the right BLA rsFC with left PCC, right HIPP and bilateral INS/putamen decreased significantly [21]. The acupuncture with Deqi group showed rsFC increased in the ACC subregion of the right supplementary motor area (SMA) and bilateral PrG/postcentral gyrus (PoG) in FD patients, while rsFC in the right precuneus, middle occipital gyrus, bilateral PCC, HIPP/paraHIPP, angular gyrus and superior parietal lobule (SPL) decreased after 4 weeks treatment [26].
After 2 weeks of MA treatment in FC patients, the ALFF values of brain regions in the Default Mode Network (DMN), such as right HIPP and left superior parietal gyrus, and the Salience Network (SN), such as the right anterior insula and left ACC increased. While the ALFF values in the DMN regions, such as left superior parietal gyrus, right superior temporal gyrus, left middle temporal gyrus and left supramarginal gyrus decreased [30]. Two weeks after treatment, the MA group showed that the functional connectivity of the left PCC (IC2), left precuneus (IC5), right superior temporal gyrus (IC25) and right cuneus (IC26) within the DMN was enhanced [31]. After MA treatment in patients with FC, the functional connectivity between the left HIPP and the right inferior frontal gyrus triangle, bilateral insula, and right inferior frontal gyrus was enhanced [32].
Event-related fMRI before and after acupuncture treatment
After 4 weeks of EA treatment, the activation voxel values of ACC, right insular cortex (IC) and PFC brain regions decreased in IBS-C patients under 150 ml colorectal dilatation (CRD) stimulation [27], while only the activation voxel values of PFC brain regions decreased in IBS-D patients under 150 ml CRD stimulation [29]. During (15 min) and immediately (30 min) after EA, the brain activation of ACC, bilateral PFC, thalamus, temporal regions and right insula increased [28].
The inconsistent results of these several studies may be due to different disease types (FD or IBS or FC) of FGIDs patients, intervention measures (MA or EA or taVNS), acupuncture points, and the duration or number of treatments.
Comparison between acupuncture and sham acupuncture or no intervention groups
Compared with the sham-taVNS control group, the ALFF values of the left inferior temporal gyrus, left paraHIPP, left HIPP, left orbital inferior frontal gyrus, left insula, left superior temporal gyrus temporal pole, left fusiform gyrus and left middle gyrus temporal pole in the taVNS treatment group of FD patients increased (P < 0.05) [23]. Compared with the group without obvious Deqi, the left BLA rsFC with bilateral INS, putamen and middle/posterior cingulate cortex (MCC/PCC), right pallidum and HIPP in the obvious Deqi group of FD patients decreased significantly after treatment [21]. Compared to the actual Deqi group, the actual without Deqi group showed significantly increased right 17(ACC subregion) rsFC with right cerebellum after treatment.There was no significant difference in left 17 and bilateral S2 rsFC between the two groups of FD patients after treatment [26]. Compared with sham acupuncture, the activation of the right insula, pulvinar and medial nucleus of the thalamus in IBS patients in the EA group was significantly increased [28]. Compared to the WT group, FC patients in MA group showed increased functional connectivity in the left PCG (IC2) and right precuneus (IC25), and decrease in the left supramarginal gyrus (IC5) and left cuneus (IC26) after treatment [31]. After treatment of FC patients, the functional connectivity of left HIPP and inferior frontal gyrus of MA Group were greater than that in WT Group [32].
Comparison between acupuncture and moxibustion groups
Compared with acupuncture and moxibustion after Zusanli (ST36) treatment of FD patients, the brain area with acupuncture higher than the fALFF value of moxibustion was mainly right putamen (P < 0.01), and the brain area with lower fALFF value was mainly mid-occipital gyrus (P < 0.01) [25]. In the study of Chu et al [27] and Zhao et al [29], there was no significant difference in the activity of ACC, left IC,right IC, and PFC between the EA group and the MOX group, regardless of whether they were IBS-C or IBS -D patients(P>0.05).
Comparison between acupuncture and medication groups
Compared with Polyethylene glycol (PEG) treatment, the ALFF value of left PCC in FC patients was significantly increased after MA treatment [30].
Methodological quality
The risk of bias and methodological quality assessment of the included studies are shown in Fig. 4. (1) Selection bias: All included studies were RCTs, of which 8 studies [21, 25,26,27,28,29,30,31,32] used the “random number table” or “computer-generated random” method to generate random sequences, and only one study [23, 24] mentioned the word “random”, so it was evaluated as “unclear”. The allocation concealment method of four studies [25, 27, 29, 30] was sealed in envelopes, and the remaining six studies [21, 23, 24, 26, 28, 31, 32] did not mention the specific concealment method. (2) Performance bias: A proportion of studies [25, 27, 29,30,31,32] used non-acupuncture controls, such as moxibustion or oral medication, which can clearly detect the treatment method and judged as “high risk”. (3) Detection bias: Only one study [23, 24] showed that doctors, subjects, data collectors, and data analysts were all blinded, and none of the other studies described whether blinding was used in the evaluation of outcome indicators, so they were judged as “unclear”. (4) Attrition bias: Six studies [21, 25, 27, 30,31,32] reported case dropout and specific reasons for dropout, but no intentionality analysis was performed when reporting the outcome, so it was judged as “high risk”. (5) Reporting bias: Two studies [23, 24, 28] did not mention clinical trial registration, so they were judged as “high risk”. One study [25] did not provide exact clinical trial registration information, so it was judged as “unclear”. (6) Other bias: All studies found no significant other biases.
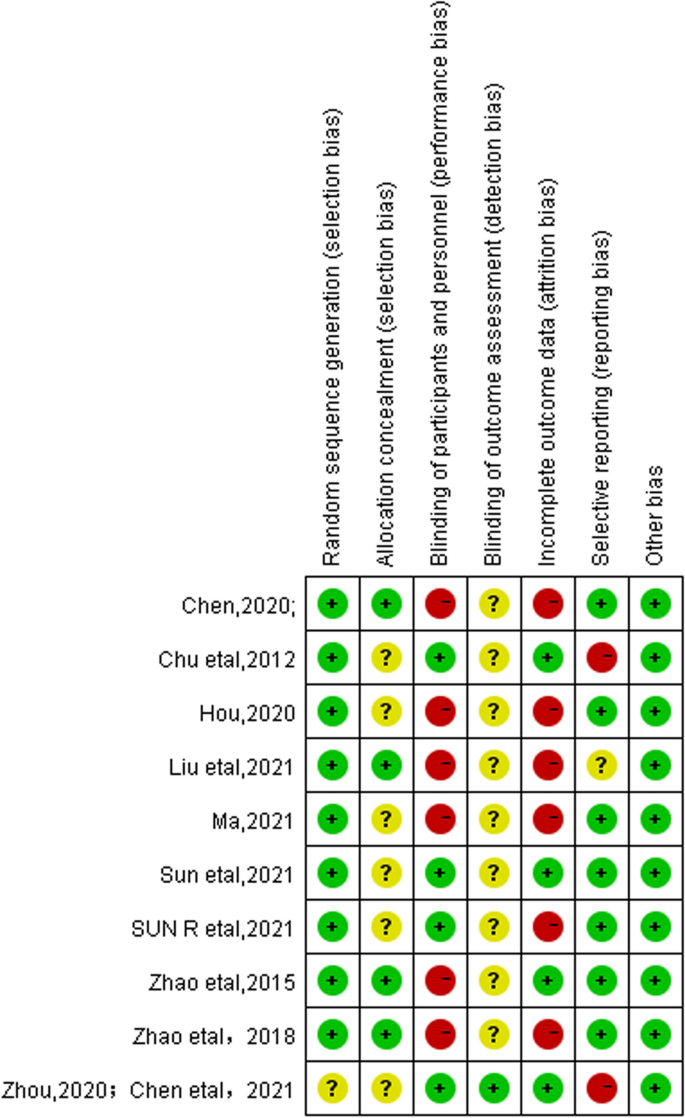

Assessment of the risk of bias of each included trial
Green: Low risk of bias; Yellow: Unclear risk of bias: Red: High risk of bias