The stigma surrounding mental health has decreased significantly in the United States, meaning more people than ever before can access treatment. But other barriers, such as a shortage of mental health professionals, continue to prevent people from seeking help. According to the U.S. Department of Health and Human Services, more than one in 10 Americans lack adequate access to mental health care.
ADHD Advisor used data from the U.S. Health Resources and Services Administration to map and analyze mental health provider shortages across the U.S. Underserved areas are considered those with fewer than one provider for every 30,000 people, or a provider shortage of 1:20,000 in high-need communities. While this analysis focuses on geographic shortage areas, other designations may impact certain demographics or facilities, such as prisons.
Lack of access to mental health care can have long-term effects across the United States, leading some to go without a proper diagnosis or turn to drugs and alcohol to self-medicate. Even for those who are diagnosed, including those with ADHD, inadequate access to mental health care can prevent them from seeking help or properly managing their medications. This is especially true in rural counties, where existing limited access to care, including long wait times and long distances to travel for treatment, has been further hindered by the COVID-19 pandemic.
Mississippi has nine designated geographic mental health shortage areas spanning 70 counties. Approximately 911,600 underserved residents, or 31.0% of the state’s population, are in the state. Read the national analysis to learn more.
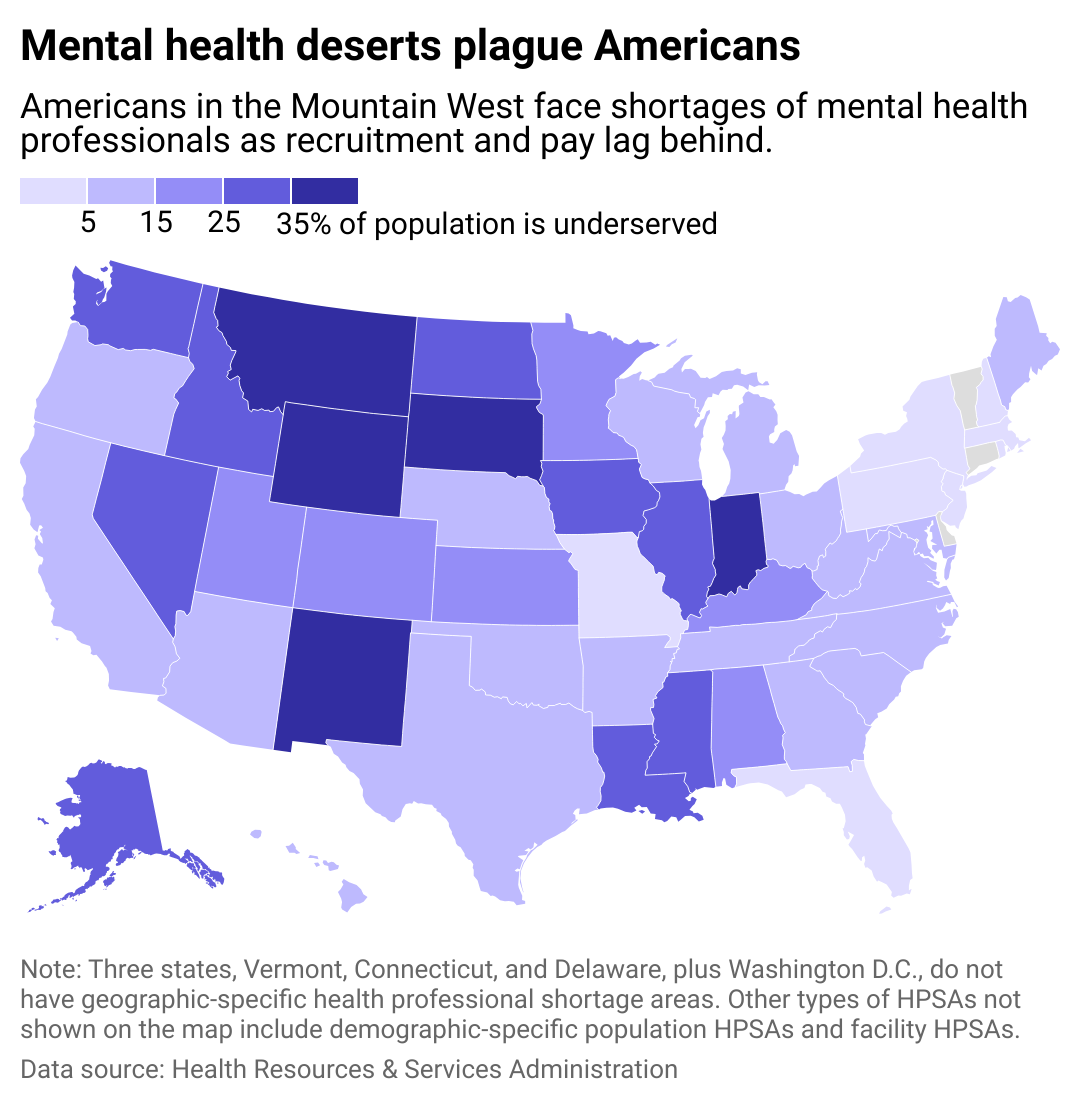
ADHD Advisor
Five states have more than 35% of their population underserved
The shortage of mental health providers is affecting people in communities across the United States, with South Dakota, Wyoming, New Mexico, Indiana and Montana facing the most severe shortages.
It’s a continuous vicious cycle. A shortage of health care workers means doctors and clinicians are shouldering huge caseloads, which can lead to burnout and increased turnover. In New Mexico, for example, the Centers for Disease Control and Prevention estimates the state needs at least 61 mental health professionals to ease the strain, but low wages make it difficult to recruit from outside the state.
Lawmakers at the local and federal levels are working together to try to improve the situation.
The Biden administration is pumping billions of dollars into improving access to care, including grants to increase the supply of mental health professionals in high-need areas. States are also playing an active role by offering financial incentives, including student loan repayment. Apprenticeship programs could also help stem some of the talent shortage in high-need areas. In Alabama, for example, students earning a master’s degree in social work at the University of Alabama can gain real-world experience while still getting paid.
While there’s no one-size-fits-all approach to solving the mental health crisis, its effects are being felt across the country: In 2020, Americans spent about $280.5 billion on mental health and substance abuse treatment, with about a quarter of that covered by Medicaid spending alone.
This story features data reporting by Elena Cox and Paxtin Marten, writing by Elena Cox, and is part of a series on leveraging data automation across 47 states.
This story originally appeared on ADHD Advisor , produced and distributed in partnership with Stacker Studio.

