Demographic characteristics
Table 1 provides basic demographic details of the study participants.
According to Table 1, most of the study participants were female, 57% (n = 62), and 42% (n = 46) were male. The age range of participants was 21 years to 65 years, with a mean age of 33 (SD = 7.9) years, and the majority (80% (n = 87)) were younger than 40 years. Almost half of the participants, 46% (n = 50), were from Blantyre. Most respondents 77% (n = 84) were from Blantyre and Lilongwe city referral hospitals, while only 23% (n = 25) were from Mangochi and Karonga district hospitals .
The prevalence of depression, anxiety, and PTSD related to COVID-19
Table 2 shows the prevalence of COVID-19-related depression in points, separated by demographic factors.
The results of this study (Table 2) showed an overall high prevalence of COVID-19-related depression (31%; CI [23, 41]), anxiety (30%; CI [22, 40]) and PTSD (25%; CI [17, 34]) among healthcare workers. However, as highlighted in Figure 1, most respondents had mild depression (18.4%) or anxiety (20.2%).
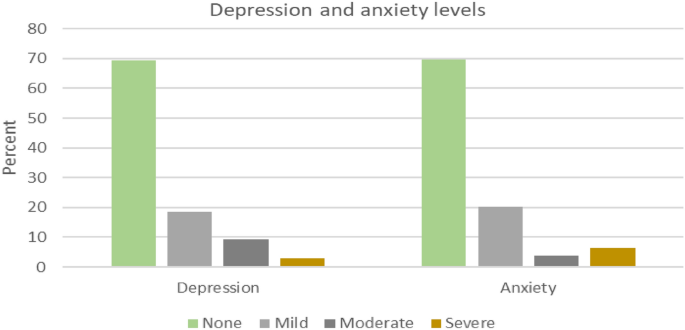
Levels of depression and anxiety among sampled healthcare workers.
High rates of depression were observed in Blantyre (n = 20, 40%) and female health workers (n = 24, 39%). On the other hand, higher rates of anxiety were observed in Lilongwe (n = 15, 44%) and female health workers (n = 22, 35%). Additionally, high rates of she-PTSD incidence were observed in Lilongwe (n = 12, 35%) and female health workers (n = 18, 29%).
Although differences were observed in the prevalence of depression, anxiety, and PTSD across different variable groups, regression results revealed that these differences were not statistically significant (Table 3 ).
Qualitative data analysis revealed three main themes that summarize the experiences and challenges faced by healthcare workers in Malawi during the COVID-19 pandemic. 1) mental health symptoms and psychological distress, 2) impact on work and personal life, and 3) stigma and discrimination.
Mental health symptoms and emotional distress
Health workers in the four districts reported experiencing a range of concerning mental health symptoms related to depression, anxiety and post-traumatic stress disorder (PTSD). When it comes to symptoms of depression, many workers report persistent sadness, feelings of hopelessness, loss of interest in daily activities, fatigue, feelings of worthlessness or guilt, difficulty concentrating, and repeated thoughts of death or suicide. I am expressing my thoughts on this. Health care workers cited excessive worrying, restlessness, difficulty relaxing, irritability, muscle tension, sleep problems, and panic attacks as symptoms associated with anxiety. Additionally, workers reported symptoms associated with PTSD, including unwanted and painful memories of treating COVID-19 patients and emotional and physical reactions when recalling traumatic pandemic experiences. This avoidance of people and situations causes reminiscences of the trauma, hypervigilance, and an exaggerated startle response. “Most of us were haunted by memories of deaths from COVID-19. We could barely sleep through the night. Several health workers reported the same to me. They came to me for help, but all I could do was give them sleeping pills.” (Matron, Karonga). “Sometimes I wish we could just shut down and forget about it all. It was too hard for us. It was too sad.” (Matron, Lilongwe).
Health workers described these mental health symptoms as having been present for several months since the onset of the COVID-19 pandemic and had a significant impact on daily functioning and quality of life. Some workers reported being unable to get out of bed in the morning due to depression, while others reported having difficulty concentrating on work due to high anxiety. The intrusive act of re-experiencing PTSD symptoms was causing great distress for some workers. Several workers tearfully recalled traumatic events, including holding the hands of dying coronavirus patients. These traumatic memories haunt health care workers, causing sleep disturbances and psychological distress. Additionally, traumatic experiences related to caring for COVID-19 patients also triggered her PTSD symptoms, including intrusive memories and emotional numbing. A nurse in Lilongwe said:I can still hear the ventilator alarm and see the faces of the patients who died. It’s like a constant reminder of the tragedy we witnessed.”
In addition to related symptoms, healthcare workers also said they were experiencing severe psychological distress from experiencing rapid deterioration and death in patients infected with COVID-19. One clinician in Mangochi district spoke poignantly: “Many medical professionals say they are used to such things, but with that disease, it is not easy for a person who had been fine until now to suddenly develop the disease, worsen, and suddenly die. ” (Clinician Mangochi). In addition, anxiety symptoms are also prevalent, with health care professionals mentioning excessive worrying, restlessness, and sleep disturbances. A clinician from Karonga province said:I lay awake at night, my mind racing with all the patients I couldn’t save and the constant fear of bringing the virus home to my family.”
These clinician testimonies provide insight into the trauma and moral injury that the severe severity and frequent fatalities of COVID-19 have inflicted on health care workers. This exemplifies the psychological impact of directly experiencing the rapid decline and death of a patient, sometimes without sufficient resources to prevent the devastating outcome. The sentiments expressed by this frontline worker in Mangochi district were echoed by many others struggling to come to terms with the sudden loss of a patient’s life. One nurse from Karonga province said:Despite our best efforts, we felt so overwhelmed and helpless as we watched our patients deteriorate.It was like a never-ending nightmareThese experiences likely contributed to the high burden of depression, anxiety, and PTSD symptoms endorsed by healthcare workers during Malawi’s COVID-19 response.
Impact on work and personal life
Participants reported that front-line health workers are overwhelmed by the increasing number of patients and the reduced number of health workers. However, in Mangochi, respondents reported an overall decline in the number of cases, from about 60 to 30 per day. This did not lead to a reduction in workload, as there was also a reduction in the number of healthcare workers due to various reasons such as unexcused absences, illness, and transfers. One of Mangochi’s nurses said:We were stretched thin, working endless hours with little rest. It was physically and mentally draining. ” The same was true in Karonga province, where health workers were required to work for two consecutive weeks and then take a week off. This work overload may have contributed to “burnout” as reported by most participants. “As you know, the workload has increased. The pandemic, especially the second wave, hit us hard, so the workload suddenly increased” (Karonga nurse).
Respondents also reported a reduction in face-to-face interactions with colleagues, primarily due to new work procedures. COVID-19 precautions, such as social distancing and frequent use of personal protective equipment (PPE), have reduced people’s sense of connectedness. In addition, there was a negative impact on work output. Participants attributed this to increased absenteeism, attrition, and requests for paid time off. Participants reported that workers were more fearful of contracting COVID-19 at work during the first wave than during the second wave, as healthcare workers may have developed strategies and coping mechanisms. did. “…so there was less panic and fear in responding to the second wave because we learned what to do.” (Matron, Lilongwe) Additionally, the fear of contracting the virus and infecting loved ones has also taken a toll on healthcare workers’ family relationships. ”I had to isolate myself from my family for months, unable to hug and comfort my children when they needed me most.it was a painful sacrifice” (Clinician, Blantyre).
The COVID-19 pandemic has also disrupted health care workers’ family relationships and social connections in many ways. Many participants spoke of their constant fear of spreading the virus to their loved ones. This has led some workers to struggle with completely isolating themselves from their families to avoid possible infection. One of the dorm mothers in Lilongwe explained: ”There were times when I thought I should send my wife and kids home and be alone.“At an already stressful time, sacrificing this important family bond caused deep emotional distress and left workers feeling isolated at a time when they needed support most. Even for those who have died, the fear of contracting the virus has strained family dynamics, with workers reporting emotions such as hugging loved ones and attending important events such as weddings and funerals. Medical workers also expressed that not being able to feel safe about their health is taking a toll on their mental health due to this constant stress and distance from their relationships, as well as the loss of colleagues and team morale. Influence.”Losing a colleague to COVID-19 was devastating.It felt like a part of my family was gone, and the emptiness they left behind was immense” (Nurse from Karonga Province).
prejudice and discrimination
Health workers faced significant prejudice and discrimination from the community because of their profession. Many cases of social isolation, harassment, and even violence have been reported. One of Mangochi’s nurses said:People called me a virus carrier and yelled at me on the street. They swerved across the road to avoid passing me as if I were a walking biohazard.“The stigma extended to their living conditions, with some health workers forced out of their homes by their landlords for fear of spreading the virus.”I was kicked out of my rented apartment because my landlord found out that I was working in a COVID-19 ward.I had nowhere to go and felt completely betrayed.” (Nurse, Lilongwe).
Participants spoke of widespread prejudice from the community that damaged their social lives and self-esteem. Many health care workers felt alienated from the communities they were trying to serve. Friends and neighbors avoided interacting with them in public for fear of infection. This social stigma has made healthcare workers increasingly isolated from traditional social supports. For some health workers, the stigma escalated to threats of physical violence. Reports surfaced of local residents throwing stones at visiting health workers or preventing them from entering villages to administer vaccines. Workers feared the aggression was caused by misinformation linking them to the virus. The social rejection, housing discrimination, and violence that participants described demonstrate the psychological toll of prejudice during a public health crisis. Healthcare workers were hurting and fearful in the very communities they sacrificed to protect. The abuse exacerbated an already isolating and stressful pandemic working environment.
Many healthcare workers experienced self-stigma and were reluctant to seek mental health support, even though several psychosocial support services were available. They feared further criticism from colleagues who might view them as weak or unable to fulfill their job responsibilities. A Blantyre clinician admitted: ”I was afraid to admit that I needed mental health support.I didn’t want my co-workers to think I was weak or incapable of doing my job.“In addition to fear of being stigmatized, many workers were unaware of the existence of in-house counseling and support services; and due to heavy workloads, even if they knew they were available, However, I had very little time to use such services.