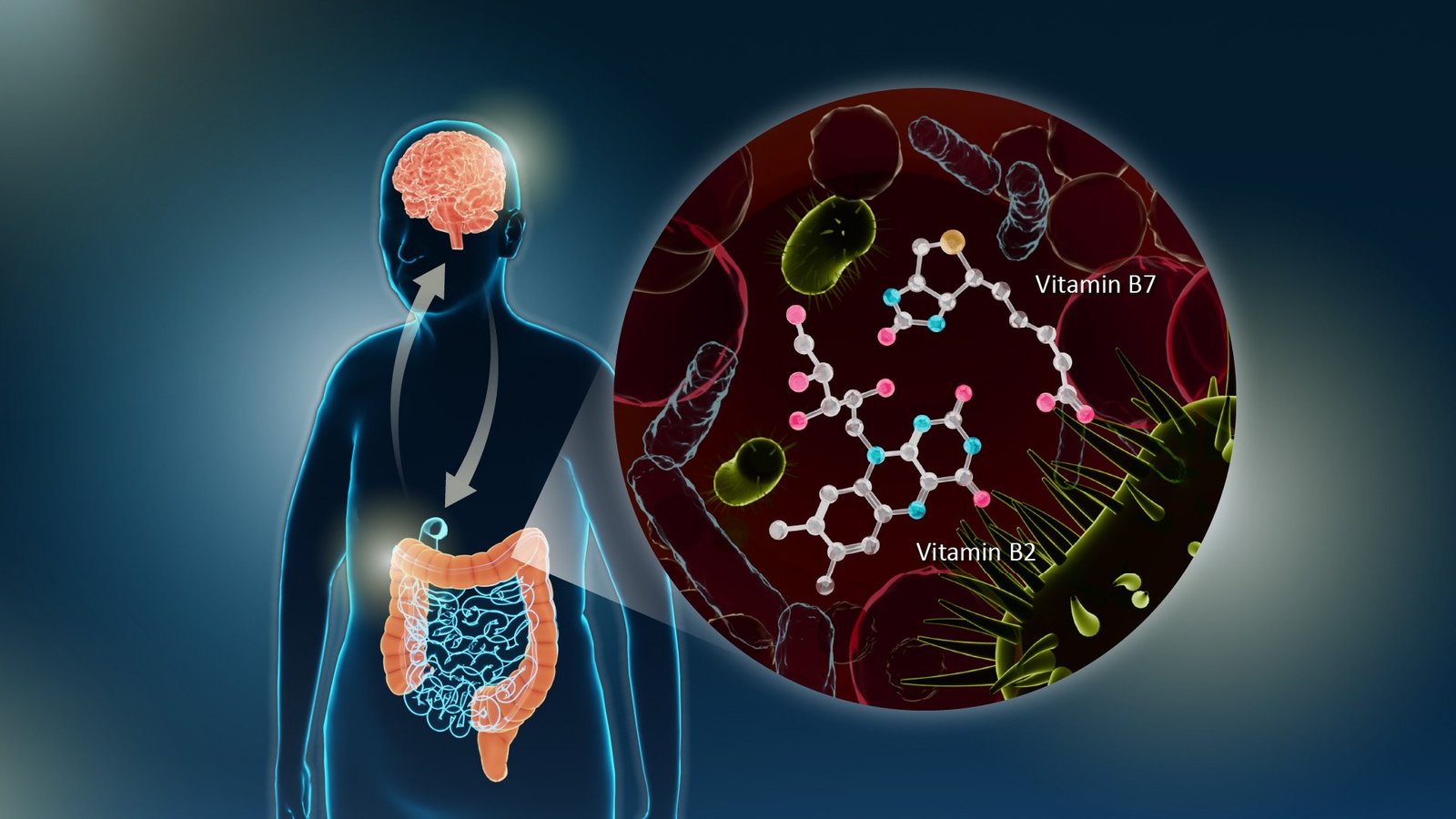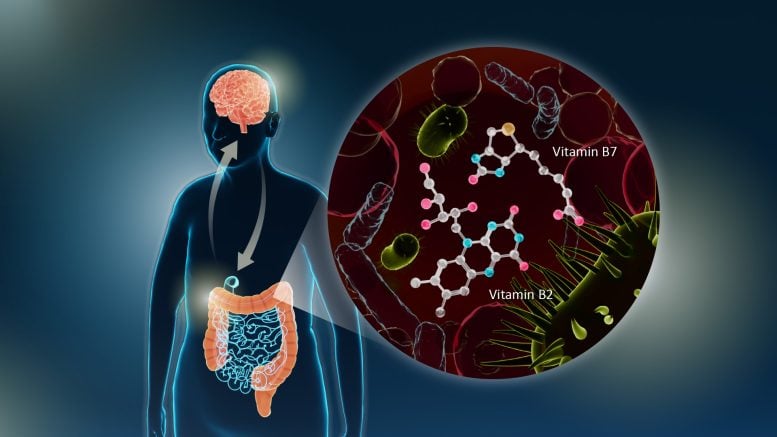
In Parkinson’s disease, the genes responsible for the synthesis of the essential B vitamins B2 and B7 were found to be reduced in gut bacteria. Photo courtesy of Reiko Matsushita
Nagoya University Researchers found that deficiencies in gut bacterial genes for vitamins B2 and B7 were associated with Parkinson’s disease, suggesting that vitamin B supplementation may be a potential treatment.
A study conducted by the Graduate School of Medicine at Nagoya University in Japan has uncovered a link between gut microbiota and Parkinson’s disease (PD). The researchers observed a decrease in gut bacterial genes responsible for the synthesis of essential B vitamins B2 and B7. They also found an association between defects in these genes and reduced levels of factors that help maintain the integrity of the intestinal barrier.
This barrier prevents toxins from entering the bloodstream and causing the inflammation seen in PD. npj Parkinson’s diseasesuggests that treatment with B vitamins that address these deficiencies could be used to treat PD.
PD is characterized by a variety of physical symptoms that interfere with daily activities and mobility, including tremors, slowness of movement, stiffness, balance problems, etc. The incidence of PD varies across populations, but it is estimated to affect approximately 1-2% of people aged 55 years or older.
Various physiological processes are heavily influenced by the microbes that live in the gut (collectively known as the gut microbiota). Under ideal conditions, the gut microbiota produces short-chain fatty acids and polyamines and maintains the intestinal barrier that prevents toxins from entering the bloodstream. Toxins in the blood can then be transported to the brain, where they can cause inflammation and affect neurotransmission processes that are essential for maintaining mental health.
Research Process
To better understand the relationship of gut microbial characteristics in Parkinson’s disease, Professors Hiroshi Nishiwaki and Jun Ueyama of the Nagoya University Graduate School of Medicine conducted a meta-analysis of stool samples from Parkinson’s disease patients from Japan, the United States, Germany, China, and Taiwan. They used shotgun sequencing, a technique that sequences all the genetic material in a sample, which is an invaluable tool because it allows for a deeper understanding of the microbial community and genetic makeup of the sample.
The researchers found that bacterial genes responsible for the synthesis of riboflavin (vitamin B2) and biotin (vitamin B7) were reduced in patients diagnosed with PD. Riboflavin and biotin, available from both food and the gut microbiota, have anti-inflammatory properties and may reduce the neuroinflammation seen in diseases like PD.
The role of vitamin B
B vitamins play a key role in metabolic processes that affect the production and function of short-chain fatty acids (SCFAs) and polyamines, two substances that maintain the integrity of the intestinal barrier and prevent toxins from entering the bloodstream. Examination of fecal metabolites has revealed a decrease in both in PD patients.
The findings point to a potential explanation for the progression of Parkinson’s disease: “A deficiency in polyamines and short-chain fatty acids may lead to a thinning of the intestinal mucus layer and increased intestinal permeability, both of which have been observed in Parkinson’s disease,” Nishiwaki explained. “This increased permeability exposes neurons to toxins and contributes to the abnormal aggregation of α-synuclein, activating immune cells in the brain and leading to long-term inflammation.”
“Supplementation targeting riboflavin and biotin holds promise as a potential therapeutic avenue to alleviate Parkinson’s disease symptoms and slow disease progression,” he added.
The findings highlight the importance of understanding the complex relationship between gut microbiota, metabolic pathways, and neurodegeneration. In the coming years, it may be possible to customize treatments based on each patient’s unique microbiome profile. By modifying the levels of bacteria in the microbiome, doctors may be able to delay the onset of symptoms associated with diseases such as Parkinson’s.
“We could conduct gut microbiota analysis and fecal metabolite analysis of patients,” Nishiwaki says, “and use these results to identify individuals with specific deficiencies and potentially create effective treatments by administering oral riboflavin and biotin supplements to those with reduced levels.”
Reference: “Meta-analysis of shotgun sequencing of gut microbiota in Parkinson’s disease,” by Hiroshi Nishiwaki, Jun Ueyama, Mikako Ito, Tomonari Hamaguchi, Keiichi Takimoto, Tetsuya Maeda, Kenichi Kashiwara, Yoshio Tsuboi, Hiroshi Mori, Takeshi Kurokawa, Masahisa Katsuno, Masaaki Hirayama, and Kinji Ohno, May 21, 2024; npj Parkinson’s disease.
DOI: 10.1038/s41531-024-00724-z