Dr. Jones: Approximately 85% of menopausal women experience hot flashes, and approximately 1 in 7 women feel that hot flashes significantly interfere with their daily life. And not everyone can or wants to take advantage of prescription therapy. So what are the other options for getting your life back?
I’m Dr. Kurtley Jones from the Department of Obstetrics and Gynecology at Utah Health University. Let’s talk about some non-medical approaches to hot flashes.
And here to help us is Dr. Lisa Taylor Swanson. She earned her Ph.D. and is a licensed acupuncturist. She is an assistant professor of health systems and community-based care in the College of Nursing and an adjunct professor of obstetrics and gynecology at the University of Utah School of Medicine. Thank you for helping me out with the long line, Lisa.
Dr. Taylor Swanson: You’re welcome, Kirtley. With pleasure. Thank you for inviting me.
Understanding complementary and integrative medicine
Dr. Jones: So let’s start a little bit. . . Complementary and integrative medicine are terms that resonate with many women seeking help for menopausal symptoms. They see themselves as whole women, not just hot flashes. So what do these terms mean? Please help me with that.
Dr. Taylor Swanson: Honestly, these terms have changed over time. So in his 20, 25 years of practicing East Asian medicine, which includes acupuncture, and his 10, 15 years of doing research, things have changed from complementary to health integrative medicine terminology. It has changed to something that is used more and more. .
And I think this shows a recognition that a lot of people are using these treatments. Both in terms of seeing a health care provider like me or a massage therapist receiving an acupuncture treatment, and also in terms of using it for self-care. .
So I think the word complementary is like, “Oh, it’s set aside. It’s like a little sister.” Actually, “integrated health” is a somewhat newer term.
But I would say that I hope that in the next few years things move toward integrated care, where there’s actually communication between health care providers and electronic medical records can be shared. So we really integrate pharmaceuticals, hormone therapy, herbal therapy, massage therapy, etc. to really provide whole-person care in an integrated way. It’s really fragmented now.
Dr. Jones: I think that’s what patients really want. They want to be seen as whole people, but they also want their caregivers to talk to each other. And I think that’s really important.
Acupuncture is a safe and effective treatment for hot flashes
Well, you’re a licensed acupuncturist. Can you talk about acupuncture and hot flashes?
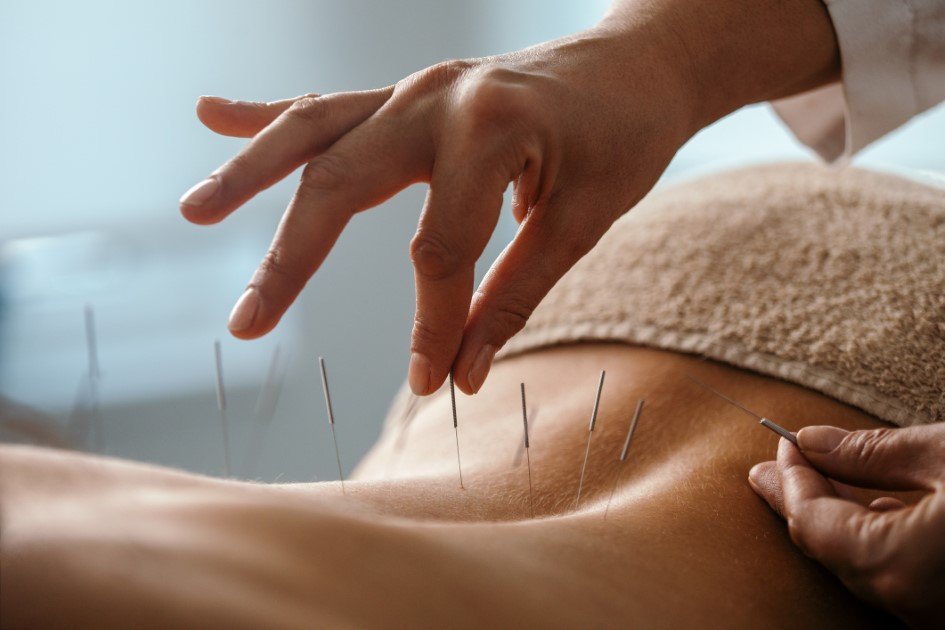
Dr. Taylor Swanson: Well, I have a few things to say. One is safety. As a treatment, acupuncture is a very safe intervention. It’s worth considering. It has also been proven to be effective. Effective for hot flashes.
Without getting too into the topic, most of the studies that have been done to date have compared acupuncture to conventional treatment and have found large effect sizes. It is much more effective than regular care.
However, when acupuncture is compared to sham acupuncture, the effect size is statistically smaller. But that’s because fakes aren’t fakes. It’s not inert, so it’s honestly a flawed design. Again, this is about research. But what I can say with complete confidence is that it is very safe and effective and definitely worth considering.
Dr. Jones: So fake acupuncture becomes something of a thing. . . Well, not really, but it’s kind of the equivalent of a placebo in terms of the pill type of research.
But there’s a sense that there’s something about that therapeutic relationship, that therapeutic touch, and people’s own inner doctors who want to make people feel better. And that’s really important. You still have to take steps to get treatment or get help from someone in your space. And you have to believe that you are strong enough to get better.
Now, given that hot flashes last for years, how many sessions do I need? Do I have to continue acupuncture for years, just like with hormone therapy?
Dr. Taylor Swanson: Well, the good news is, no, it won’t last for years. The literature shows that women in very large randomized controlled studies said, “Oh, this was the biggest improvement they were going to experience,” after eight sessions a week. It’s very clear that we’re going to end up in some kind of stagnation. Therefore, I always encourage women to consider eight sessions per week. In reality, all you have to do is sign them up for weekly care for two months and see how they feel.
But getting back to the whole person topic, what I want to say is that what I’ve seen many times in my own practice is that typically after 3, 4, or 5 sessions a week, patients also… And I was like, “Wow, they feel so much better.” Of course I’m going to continue to work on my hot flash symptoms.
But you might also say, “Oh my god, my lower back hurts so much,” or “I have migraines, too.” And typically, yes, with eight sessions a week, you’ll see an improvement in your hot flashes, but perhaps you can also start working on other things that will improve both of you together. It’s very exciting.
Dr. Jones: Oh, that’s what you have to say when starting with estrogen. . . Hormone replacement therapy does improve joint pain for some people, and for others it also improves insomnia and other symptoms.
But they don’t always have time with me. Even if my therapeutic touch is good, if it only takes 5 or 10 minutes of their time with me, I know I’m really providing the type of “let’s do this together” session that they think they’ll like. I can’t say. And worth it.
Menopause has many symptoms, aging has many symptoms, and women are looking for an integrated approach to all of them. They don’t want you to say, “I’ll come to you for this and I’ll come to you for that.” However, you and your group have started a new approach for women and named it MENOGAP. Can you help me think about it?
MENOGAP: Closing the gap in menopause care
Dr. Taylor Swanson: MENOGAP therefore has a dual purpose. One is that we organized this group medical visit to fill a gap in health care for menopausal women. And that is also what we are providing with the biomedical care provided by my esteemed colleagues, primarily Camille Moreno.
Dr. Moreno and I work together. We are an integrated team. That’s why we talked earlier about integrated care, and it’s easy to talk about it.
It also means GAP, or menopausal care through group acupuncture.
So what we do there is provide top-of-the-line care and be able to provide medical management by Dr. Moreno, who is board-certified in menopause. She provides doctor talk.
And I’ll give you some doctor talk. What is the evidence based on acupressure for self-care? Chinese herbal medicine? So I’m sure we can provide some kind of evidence, like old and new, or East and West.
And what the women literally said was, “This is the best medical care I’ve ever received in my life. It’s improved my symptoms. I feel more empowered.” I feel it.” They also know, “Oh my god, I can get menopausal hormone therapy and self-acupressure therapy.” we can do a lot together. One does not exclude the other.
Benefits of group health checkups
Dr. Jones: Now, what about group processes? Is that part of it? I think we know that for people who are able to be together socially and laugh together and be with other people, the symptoms are often burdensome. . . There may not be a dramatic change in the symptoms themselves, but I feel like the burden of my symptoms has lightened somewhat. Do you have that feeling?
Dr. Taylor Swanson: Oh boy. yes. Of course, Kirtley. In the groups we have worked with, women have not only said, I’m going crazy,” I thought, but what the woman said was even worse. . .
Especially for those who are transitioning early into perimenopause, hearing a postmenopausal colleague say, “Don’t worry, you’ll get through it. It’s actually getting better,” gave me a lot of hope. . More so than if Dr. Moreno and I had said, “Oh, don’t worry, we’ll get there.” What do we know? We’re not there yet.
But the other women in the group did. Moreover, they were able to share their expertise and share their insights with each other. It was great to hear and see in just a few weeks in weekly sessions. They really built a trusting relationship and felt comfortable sharing it knowing it was confidential and a proper medical visit, as if they were only seeing either Camille or me. .
CULTURAL INCLUSION IN MENOGAP
Dr. Jones: Well, our community is becoming more and more diverse both culturally and racially, but I don’t even want to say racial because I don’t know what that means genetically anymore. But how do you get people from different backgrounds into a room?
Dr. Taylor Swanson: This comes naturally to us because MENOGAP was developed in close collaboration with a community advisory board comprised of ethnically, racially and culturally diverse women. We had a community of women who said, “Yes, let’s work on this together.”
So the intervention itself included, for example, African American black CAB members saying, “Oh, we should do this.” We had one Native American woman, two Latinas, three refugees, and a few white women. And everyone worked together to provide input on what this intervention should be.
So this was really designed from the beginning with inclusivity in mind, and the main common denominator in delivering the MENOGAP intervention is respect.
And I’ll also briefly mention that there are two other teams working to put sophisticated mindful adaptations of MENOGAP into practice. One of them is designed by and for Indigenous women. So Indigenous women, both on the team and in the community, have further applied her MENOGAP and are calling it the Waning Moon. It’s a collaboration with the Urban Indian Center in Salt Lake.
And another team that Camille and I work with is also made up of Latina and Hispanic women. And we plan to pilot test it soon with members of our community. It’s about adapting it to Spanish for delivery to local health workers. And that is Mujeres en la Transción. My Spanish isn’t very good, sorry. But “women in transition.”
How to participate in MENOGAP
Dr. Jones: That’s really great. And how can women find out more and register?
Dr. Taylor Swanson: Well, maybe you could look me up at the University of Utah or Camille. You can also email menogap@umail.utah.edu.
Dr. Jones: That’s MENOGAP from the University of Utah. Are there any other MENOGAPs? Is this just local? . . Are we the first and the best? Okay, fine.
Dr. Taylor Swanson: All over the world, I might say Kirtley.
Dr. Jones: All over the world, yes. Join the new wave of caring for women as a group. Let’s be considerate of each other and help each other. Thank you, Lisa.
And if you know someone who suffers from hot flashes, midlife or menopause symptoms, or who is looking for a non-medical approach, we invite you to join the MENOGAP program. Sometimes it takes a village, a community of women, to find your way.